This week was filled with patients with some challenging diseases, none more so than megaesophagus! What’s that you ask? Please take a few minutes to read more about this potentially debilitating disease of the esophagus (food tube) below.
What is megaesophagus?
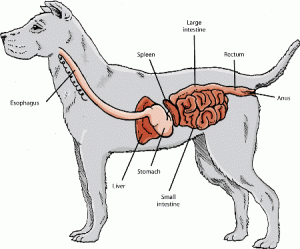
Megaesophagus is a condition where there is decreased or absent muscular contractions of the esophagus, the tube that carries food and water from the mouth to the stomach. Patients with this disease have difficulty passing food all the way to the stomach, and food subsequently may be regurgitated. This reduced motility usually results in dilation of the esophagus.
(Illustration courtesy of The Merck Manual for Pet Health)
Megaesophagus may be present at birth or can be acquired later in life. It can be secondary to a variety of diseases that cause esophageal nerves and/or muscle to improperly function, including:
- Infectious disease (i.e.: canine distemper)
- Esophageal obstruction
- Esophageal stricture
- Esophageal cancer
- Compression by a mass in the chest cavity (i.e.: thymoma)
- Compression by a congenital defect of the blood vessels in front of the heart
- Inadequate function of the adrenal glands (Addison’s disease)
- Myasthenia gravis (an disorder of the immune system that causes specific muscles to weaken)
- Polymyositis (inflammation of many muscles in the body)
- Systemic lupus erythematosus (aka: lupus or SLE, a disorder of the immune system)
- Botulism (type of food poisoning)
- Tetanus (bacterial infection that induces severe muscle spasms)
- Dysautonomia (inflammation and degeneration of certain components of the autonomic nervous system)
- Low thyroid hormone concentration
- Certain toxins (i.e.: lead, thallium, organophosphate)
Most commonly megaesophagus is a primary disorder with no identifiable cause (idiopathic). One should note that a primary/idiopathic condition can only be diagnosed by ruling out all possible secondary causes (see list above!)
What does a dog with megaesophagus look like?
Megaesophagus is seen in both dogs and cats, but it is much more common in the former. This condition is hereditary in the wirehaired fox terrier and miniature schnauzer.
Other commonly affected breeds are:
- German shepherd dog
- Newfoundland
- Great Dane
- Irish setter
- Chinese shar-pei
- Pug
- Greyhound
One of the most common clinical signs seen in patients with megaesophagus is regurgitation.
Remember regurgitation and vomiting are not the same!
Vomiting is an active process and regurgitation is a passive one. Cats often show signs of nausea before vomiting, and common prodromal indicators include excess salivation, licking of the lips, and vocalization / crying. During the act of vomiting, abdominal wall muscles contract to expel food and liquid from the stomach and the first part of the small intestine (duodenum). This material is called vomitus and commonly is yellow or green in color, indicating the presence of digested or fresh bile, respectively.
Regurgitation does not involve abdominal wall muscle contraction; rather it frequently occurs when a pet changes position (e.g., lowers his head). Often times parents say, “He just opened his mouth and food came out.” Regurgitus comes from the esophagus or the back of the throat (oropharynx) and often looks like a tube because of the time it spends in these locations.
My friends at the Veterinary Partner have developed a great animation to help show the difference between vomiting and regurgitation. Although the model uses a dog, the process is the same in cats. Check out this link for more information.
Other clinical signs observed in patients with megaesophagus include:
- Fever
- Coughing
- Nasal discharge
- Excessive salivation
- Difficulty swallowing
- Foul breath
- Weight loss
- Poor body condition
Affected animals often lose weight because of their inability to effectively propel food from the mouth into the gastrointestinal tract where vital nutrients are absorbed. Affected patients can also develop pneumonia secondary to regurgitation and subsequent aspiration of food into the lungs.
How is megaesophagus diagnosed?
A pet’s clinical signs are often key to making an accurate diagnosis. I strongly recommend parents video record their pet’s regurgitation at home. Remember it is extremely important to accurately differentiate regurgitation from vomiting, and a video can be invaluable! Certain blood and urine tests are necessary to both confirm the presence of megaesophagus and exclude other conditions, including:
- Complete blood count (CBC)
- Biochemical profile
- Urinalysis
- Chest radiographs (x-rays)
(The black arrows show the borders of a severely dilated esophagus; radiograph courtesy of the Comparative Neuromuscular Laboratory at the University of California – Davis)
- Acetylcholine receptor antibody titer for myasthenia gravis
- Antinuclear antibody level for immune-mediated diseases like SLE
- Hormone tesing to assess adrenal gland and thyroid gland function
- Lead level
Esophagoscopy, the use of a fibre-optic camera to visualize the inside of the esophagus, may be recommended if a patient is suspected or confirmed to be living with an esophageal foreign body, cancer or esophagitis (inflammation of the esophagus). Please see this video of a esophagoscopy in a dog.
Fluoroscopy, a form of life-action x-ray technology, allows direct visualization of the esophagus in motion to assess the strength and coordination of esophageal contractions that propel the food down into the stomach. Here’s a video of fluoroscopy in a dog.
Special testing to evaluate muscle and nerves (electromyography and nerve conduction velocity, respectively) may also be beneficial. Evaluation by a board-certified veterinary internal medicine specialist will be quite helpful in determining the most appropriate tests to perform for your pet.
How is megaesophagus treated?
The primary goals in treating megaesophagus are to:
- Identify and treat the underlying cause
- Decrease the frequency of regurgitation
- Prevent over-distention of the esophagus
- Provide adequate nutrition
- Treat complications (i.e.: aspiration pneumonia and esophagitis)
Consultation with a board-certified veterinary internal medicine specialist can be very helpful in developing a therapeutic plan for a pet with megaesophagus.
Ensuring a dog with megaesophagus eats adequate calories is of paramount importance. The most common way to feed such patients is from an elevated surface. There are many forms of elevated feeding, and the most common is an extreme form called vertical feeding. Vertical feeding is achieved using a special apparatus called a Bailey Chair, and this is the preferred method of feeding patients with megaesophagus. There are many online resources for pet parents regarding purchasing Bailey Chairs. You can even make one at home! Here’s a video of a Labrador retriever using a Bailey Chair.
If you can’t afford to purchase or make a Bailey Chair, there are alternative elevated feeding options. For example, allowing a pet to stand with the front half of the body elevated above the back half of the body (i.e.: standing on some steps) for 15-20 minutes after eating can be a very effective feeding strategy.
A high calorie diet should be fed in small amounts frequently over the course of the day to ensure sufficient intake and to decrease the likelihood of over-dilating the esophagus. We don’t know the ideal food consistency to feed patients with megaesophagus. The consistency must be tailored to each patient based on the diet that causes the fewest clinical signs.
Some pets respond better to a gruel/soup diet while others tolerate solid food better. Many accept canned food formed into small meatballs. Animals that are unable to adequately maintain caloric intake with by-mouth feedings will need a supplemental feeding tube placed into the stomach for chronic use.
Occasionally, medications that reduce stomach acid production and/or promote normal intestinal motility may be recommended. There is limited scientific evidence such drugs are effective long-term, but there is anecdotal evidence that suggests efficacy. The drug sildenafil – more commonly known as Viagra – is currently receiving a lot of attention due to its effect of the lower esophageal sphincter, the junction between the esophagus and the stomach. I’m excited to see the results of some of the studies currently underway to see if this drug may have a meaningful benefit for megaesophagus patients.
The take-away message about megaesophagus…
Megaesophagus is an often debilitating conditon of the esophagus. Accurate diagnosis is essential, as there are many diseases that can secondarily cause regurgitation and diltation of the esophagus. Consultation with a board-certified veterinary internal medicine specialist will be helpful in aiding your pet’s diagnosis and developing an appropriate treatment strategy.
To find a board-certified veterinary internal medicine specialist, please visit the American College of Veterinary Internal Medicine.
Wishing you wet-nosed kisses,
CriticalCareDVM






Christian
Thanks for the information
! You said very important things !
criticalcaredvm
Thank you so much Christian! Please help me to spread the word that pets can have specialists too!