One might think in a time when highly effective and safe vaccines for canine distemper virus are widely available this debilitating disease would be eradicated in the developed world. Sadly, that is not the case. In fact, canine distemper is still rampant in some areas of the United States. As such, this week’s post is dedicated to raising awareness of this virus and its potentially devastating effects on our canine companions. Please share with other dog owners – happy reading!

What is canine distemper?
Canine distemper – sometimes called hard pad disease – is a ribonucleic acid (RNA) virus of the Paramyxoviradiae family and Morbillivirus genus. It is highly contagious and is found worldwide. Dogs serve as the principal reservoir host, but the virus has been reports in cats, coyotes, hyenas, lions, tigers, ferrets, foxes, weasels, raccoons, seals, pandas, dolphins, and some primates.
Canine distemper virus is spread through aerosol and droplets because of its prevalence in respiratory secretions. When virus particles come into contact with cells called epithelial cells in the airway, immune system cells called macrophages engulf them and transport them to local lymph nodes. In just a few short days, the virus spreads to other lymphoid organs, particularly the spleen, lymph nodes in the abdominal cavity, and Kupffer cells in the liver. From these locations, canine distemper virus spreads via the bloodstream within 8-9 days post-infection to other cells in the epithelial cells throughout the respiratory system, gastrointestinal tract, urogenital tract, and central nervous system (CNS).
Whether a dog develops clinical signs of canine distemper depends on their immune system. If their immune system mounts an effective response within 14 days post-infection, then no clinical signs of infection may manifest. If their immune system is able to produce only a mediocre defense, then clinical signs develop, but infection should eventually be cleared. Dogs that fail to muster an immune response develop severe clinical signs and can suddenly die.
Given canine distemper virus’s ability to invade lymphoid cells, an infected dog’s immune system is markedly compromised. They experience severe immunosuppression. As such, canine distemper infection may predispose infected dogs to other infections, including those associated canine infectious respiratory disease complex.
What does it look like?
There is no breed or sex predisposition for canine distemper. Understandably, pediatric and/or unvaccinated dogs are most susceptible to disease. Manifested clinical signs depend on the robustness of the immune response an infected dog mounts. Common clinical signs observed by owners are:
- Lethargy & weakness
- Reduced (or loss of) appetite
- Discharge from the eyes and/or nose
- Sneezing
- Coughing
- Vomiting
- Diarrhea (may be hemorrhagic)
Signs involving the central nervous system include unsteadiness while walking (called ataxia), seizures, inability to walk, an abnormal muscle activity (called myoclonus and hypermetria). They can develop a few weeks after the onset of systemic signs, but may also manifest several months after an infected dog makes an apparent recovery. Please watch the video below showing a Labrador retriever puppy with focal facial seizures due to canine distemper.
How is canine distemper diagnosed?
It’s imperative veterinarians obtain a thorough patient history and perform a complete physical examination in any patient for which canine distemper infection is suspected. Physical abnormalities may include:
- Conjunctivitis
- Nasal & ocular discharge
- Fever
- Weight loss
- Dehydration
- Changes to the retina (e.g.: papilledema, detachment, scarring)
- Keratoconjunctivitis sicca (aka “dry eye”)
- Thickening & flaking of the skin on the tip of nose and paw pads (called hyperkeratosis)
- Changes to the enamel on teeth (called enamel hypoplasia)
- Ocular & nasal discharge
- Multifocal pimples (called pustular dermatitis)

In patients with compatible histories and physical examination findings, further testing is needed to confirm a clinical suspicion of canine distemper. Veterinarians will recommend the following:
- Complete blood count – evaluate white blood cells, red blood cells, and platelets
- Serum biochemical profile – to evaluate liver and kidney function, as well as electrolytes like sodium & potassium
- Radiography (x-rays) – to screen for viral pneumonia and bone changes called hypertrophic osteodystrophy
- Viral testing – samples of blood, nasal or ocular discharge, urine, cerebrospinal fluid, and other tissues can be submitted to look for inclusion bodies, measure antibodies (special immune proteins the body makes upon exposure to an infecting organism), detect genetic material of virus particles, and/or isolate the virus directly.
How is it treated?
To date there is no specific anti-viral therapy for dogs infected with canine distemper virus. Management is primarily supportive in nature. Patients may benefit from fluid therapy to correct dehydration. Those with opportunistic secondary bacterial infections should be treated with an appropriate antibiotic. Respiratory therapies, including provision of supplemental oxygen and nebulization, are often needed for those with pneumonia. Anti-convulsant medications should be used in those patients who develop seizures.
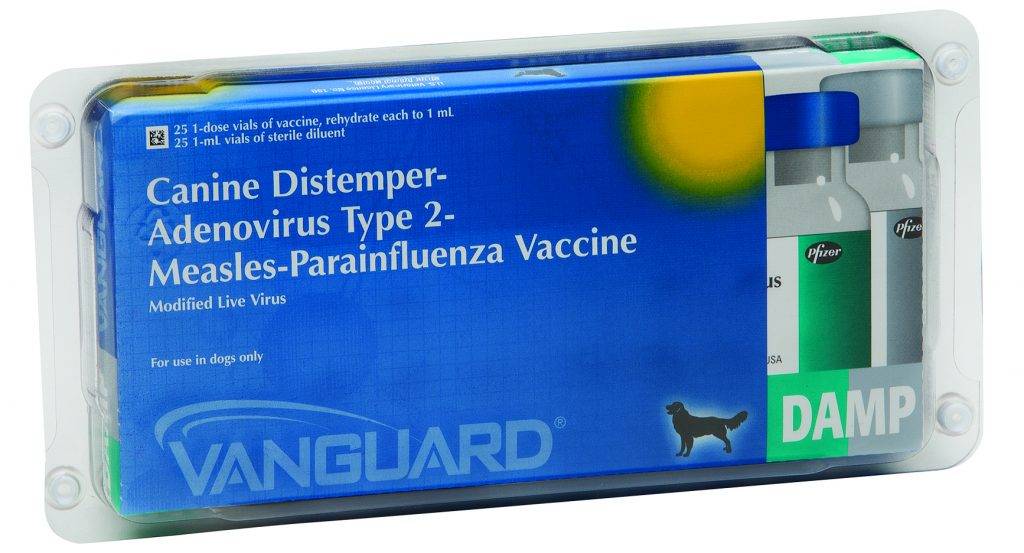
The best weapon in the battle against canine distemper virus is appropriate vaccination. The American Animal Hospital Association recommends vaccination dogs initially at 6-8 weeks of age and every 3-4 weeks after that until 14-16 weeks of age. Dogs should then receive a vaccine “booster” one year later and then every three years after that. Dogs older than four months of age at the time of initial vaccination should receive two vaccines 2-4 weeks apart. I believe it is imperative dog owners seek medical advice about which canine distemper vaccine is best for their dogs from veterinarians, not from non-veterinarian breeders or pet supply store workers who have no education, training, or experience in immunology and/or vaccinology.
The take-away message about canine distemper…
Canine distemper is a highly contagious virus that affects dogs and other animals worldwide. Clinical signs predominantly involve the respiratory, gastrointestinal, and central nervous systems. No definitive treatment is available, but prevention is possible via vaccination.
To find a board-certified veterinary internal medicine specialist, please visit the American College of Veterinary Internal Medicine.
Wishing you wet-nosed kisses,
CriticalCareDVM