Nobody likes cancer. Unfortunately, it’s a fact of life even for our furry companions. Previously, we’ve discussed lymphoma in both cats and dogs, mast cell tumors, and even anal gland tumors. This week I’m sharing information about another cancer that can affect our pets: thymoma. So, I hope you find the post interesting and share-worthy. Happy reading!

What is a thymoma?
To understand what are thymoma, you need to have a basic understanding of the anatomy of the chest. The chest or thoracic cavity has different components. Obviously, we have the rib cage, the lungs, and the heart. The mediastinum is a potential space found in the midline of the thoracic cavity that divides it into two halves. There is a front part called the cranial mediastinum, a middle part, and a back part called the caudal mediastinum.

The cranial mediastinum is the area on midline in front of the heart. This part contains the esophagus (food pipe), trachea (windpipe), and the thymus. The thymus is a small glandular organ that is a site of production and maturation of special immune system cells called T lymphocytes. This organ is very active in utero and during adolescence but regresses or involutes with age. A thymoma is a cancer arising from cells of the thymus gland called thymic epithelia.
What does it look like?
Thymoma is more common in cats compared to dogs. Any breed or sex of cat and dog can develop a thymoma, but this cancer is most commonly diagnosed in domestic shorthair cats. Thymomas arise in older pets, and the average of diagnosis in cats is 12 years of age. To date, no genetic and/or environment causes have been identified.
Pet owners often report the following clinical signs:
- Coughing
- Tachypnea (elevated respiratory rate)
- Dyspnea (respiratory distress)
- Lethargy
- Exercise intolerance
- Reduced (or loss of) appetite
- Vomiting and/or regurgitation
- Weight loss
- Inability to hold head up (called cervical ventroflexion)
- Swelling of the head, neck, and/or thoracic limbs – this constellation of clinical signs is called caval syndrome
- Muscle weakness, a dilated esophagus, and regurgitation – this constellation of clinical signs is supportive a neuromuscular condition called myasthenia gravis

How is thymoma diagnosed?
In patients with suspected thoracic disease based on their history and physical examination, veterinarians will recommend further testing, particularly imaging of the thoracic cavity. Radiographs (x-rays) can readily identify a space-occupying mass in the cranial mediastinum. However, there are other structures – most notably lymph nodes – in this location so x-rays can’t provide a definitive diagnosis. Radiographs may also identified fluid in the pleural space, a potential space between the rib cage and the lungs.
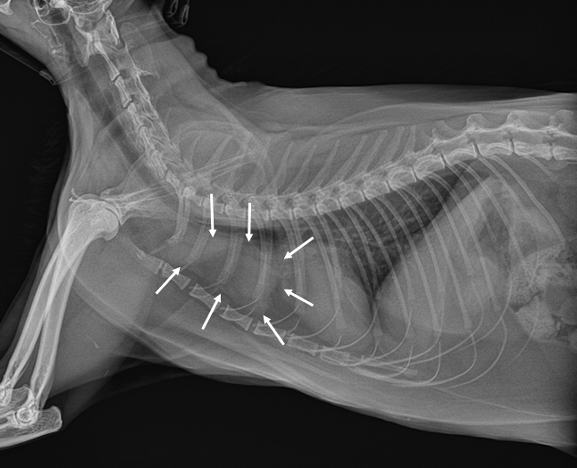
Ultrasonography – the use of ultrasound waves – can similarly identify masses in the cranial mediastinum but don’t provide a definitive diagnosis. With that being said, ultrasonography can be used to perform a minimally invasive procedure called fine needle aspiration. During this procedure, a vaccine-sized needle is guided into the mass to aspirate cells so they can be evaluated by a board-certified veterinary clinical pathologist. Computed tomography or a CT scan can be uniquely helpful as images can also be used to plan treatment like surgery and radiation therapy.
A board-certified veterinary clinical pathologist may recommend performing a special test called flow cytometry. Remember the thymus is an organ that produces T lymphocytes. Each T lymphocyte has different cell markers – think of them as hats. More than 10% of lymphocytes from thymomas express two specific markers: CD4 and CD8. In other words, thymomas tend to wear two specific hats all the time. Other cancers of the cranial mediastinum – for example, mediastinal lymphoma – don’t dually express these markers with nearly the same frequency. They wear different hats. So the degree of cell marker expression as determined from flow cytometry – aka figuring out what hats the cells are wearing – can be uniquely helpful in establishing a diagnosis.
Other tests that should be performed in pets with suspected thymomas are:
- Complete blood count
- Serum biochemical profile
- Urinalysis
- Feline leukemia virus (FeLV) – cats only
- Analysis of pleural effusion (if present)
How is it treated?
Tbe preferred treatment of thymomas is surgical removal. Depending on their size, thymomas may be removed either via thoracotomy (aka “cracking the chest”) or a minimally invasive procedure called thoracoscopy. Primary care veterinarians often refer affected patients to a board-certified veterinary surgeon. Chest surgery requires unique instrumentation and unquestionably demands skill, expertise, and fully-trained anesthesia, surgery, and critical care teams. The average survival time following surgery is 1825 days (5 years).
Surgery may not be a viable treatment option for some cats for a variety of reasons, including the tumor’s invasiveness. Indeed, degree of invasiveness is a major prognostic factor. More aggressive tumors have a poorer prognosis. In non-surgical patients, treatment with radiation therapy should be considered. This modality is well-tolerated and has been associated with an average survival time of 720 days (2 years).
The take-away message about thymoma in cats & dogs…
Thymoma is an uncommon cancer of the thymus gland found in the cranial mediastinum of cats and dogs. Common clinical signs include coughing and changes to a pet’s breathing rate and/or effort. The preferred treatment is surgery, which is associated with a meaningful survival time.
To find a board-certified veterinary oncologist, please visit the American College of Veterinary Internal Medicine.
To find a board-certified veterinary surgeon, please visit the American College of Veterinary Surgeons.
Wishing you wet-nosed kisses,
CriticalCareDVM
