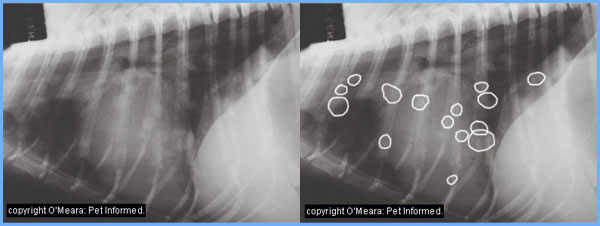
Pets, like people, can be afflicted with cancer in the lungs. Early identification is key to maximize the likelihood of a positive outcome. In an effort to increase awareness of lung tumors in our fur babies, this week I dedicate some time to explain lung cancers in dogs and cats. I hope you find the information helpful and share worthy. Happy reading!
Lung Tumors – What are they?
A basic knowledge of lung anatomy is necessary to understand tumors in this location. Dogs and cats have several lung lobes, including:
- Right cranial (toward the front of the body) lobe
- Right middle lobe
- Right caudal (toward the tail) lobe
- Left cranial lobe (divides into two segments)
- Left caudal lobe
- Accessory lobe
Cancers can start in the lungs (called primary tumors) or they can spread or metastasize to them (called secondary tumors). Primary tumors more often affect the right side. The accessory, right caudal, and left caudal lobes are over-represented for primary lung cancer because they are largest lobes. Nevertheless, metastatic disease is more common than primary tumors.
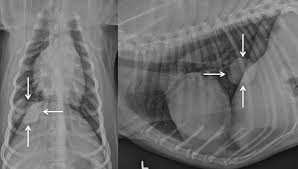
A primary lung tumor in the right caudal lung lobe of a dog (white arrows). Images courtesy of Dr. LE Barrett
The most frequently diagnosed primary lung tumor in dogs and cats is called adenocarcinoma. Less common types include squamous cell carcinoma and anaplastic carcinomas. Primary tumors that arise from connective tissue in the lungs (e.g. osteosarcoma, fibrosarcoma, hemangiosarcoma) are relative rare. Although primary tumors are statistically almost always cancerous, some benign tumors have been documented, including papillary adenoma, bronchial adenoma, plasmacytoma, fibroma, and myxochrondroma.
As mentioned earlier, secondary tumors (aka metastatic disease) is much more common than primary ones. Common tumors that like to spread from other locations in the body to the lungs include:
- Hemangiosarcoma
- Osteosarcoma
- Transitional cell carcinoma
- Mammary carcinoma
- Thyroid carcinoma
- Squamous cell carcinoma
- Melanoma
To complicate matters, primary lung tumors can metastasize to the lungs too! Therefore, a thorough diagnostic investigation is vital for accurate diagnosis.
Lung Tumors – How are they diagnosed?
Dogs and cats diagnosed with primary lung tumors are typically geriatric (more than 10 years of age). There does not seem to a breed or sex predilection; however some have reported Boxers are over-represented.
Approximately 25% of dogs with primary tumors have absolutely no clinical signs at the time of diagnosis. Only roughly 33% of cats have signs of respiratory disease. Indeed, documentation of primary tumors is frequently incidental, found as part of a preventative healthcare examination. When present, clinical signs are variable and may include:
- Non-productive cough
- Lethargy
- Fever
- Exercise intolerance
- Coughing blood
- Weight loss
- Breathing difficulty/distress
- Decreased (or loss of) appetite
If a primary or secondary lung tumor is suspected, a veterinarian will first obtain radiographs/x-rays of the chest. However, it’s important to know radiographs don’t identify all lesions as they must be approximately 0.5-1.0 centimeter in diameter to be reliably detected. Furthermore, it can be difficult to differentiate metastasis from a primary lung tumor from metastasis from a tumor in a different body organ. With that being said, primary tumors are typically discrete large focal lesions while secondary ones are smaller and multifocal.
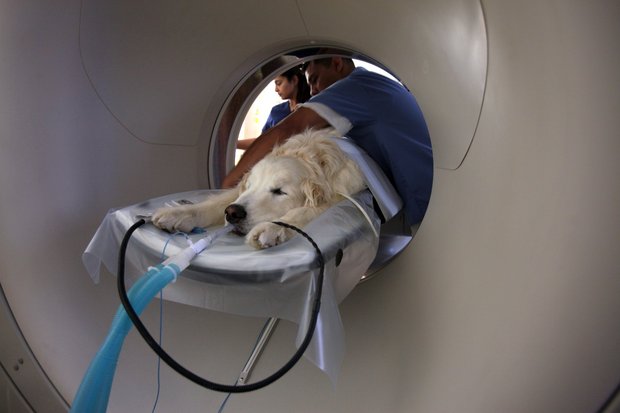
Computed tomography (CT scan) of the chest is the most sensitive imaging modality for detecting lung tumors
Your family veterinarian may refer you to a veterinary specialty hospital where advanced imaging (e.g.: computed tomography/CT scan) is available. This imaging modality is the most sensitive method for detecting lung lesions but does typically require a brief period of sedation/anesthesia.
Lung Tumors – How are they treated?
The treatment of choice for a solitary nodule(s) or multiple masses in a single lobe is surgical removal of the affected lobe as long as there is no evidence of metastasis to other sites (including other lobes). Occasionally in this scenario, your family veterinarian may refer you to a board-certified veterinary internal medicine specialist for a fine needle aspiration (FNA) of the tumor. This is a minimally invasive procedure in which a vaccine-sized needle is guided into the lesion with ultrasound technology to obtain some cells from the lung lesion. These cells are then evaluated by a board-certified veterinary clinical pathologist in an attempt to obtain a definitive diagnosis. This evaluation of cells is called cytology, and unfortunately is not always diagnostic. Thus following FNA, one faces one of two scenarios:
- Cytology identifies cancer – In this scenario, surgery will be recommended to remove the primary lesion
- Cytology does not identify cancer – Remember cytology is not always diagnostic. Not finding cancer via cytology does not mean cancer isn’t present. Thus surgery will be recommended to obtain a tissue biopsy and remove the lesion.
As you can see from the above-listed scenarios, both ultimately end with a recommendation of surgery. For this reason, some pet parents choose to forgo the FNA with cytology and elect to proceed directly with surgery after CT scanning in patients with no evidence of metastasis.
There are several techniques for removing primary lung tumors and even some secondary ones, including:
- Complete removal of an affected lobe
- Partial removal of an affected lobe
- Use of a special scope to visualize the lobe (called thoracoscopy) to obtain a piece of affected tissue through a smaller incision
As one may imagine, lung surgery is quite intricate and requires appropriate and extensive training and clinical experience. Partnering with a board-certified veterinary surgeon is invaluable for selecting the most appropriate surgical approach and maximizing the likelihood of a positive outcome. Additionally, post-operative care and monitoring for patients is exceedingly important. Patients are typically best served in hospitals that provide around-the-clock care in an Intensive Care Unit (ICU) directed by a board-certified veterinary emergency and critical care specialist.
For those patients with primary lung tumors that can’t be completely removed, as well as for for those for whom surgery is not feasible (e.g.: lung tumor is unresectable, presence of metastasis), adjuvant chemotherapy may be considered. Thankfully chemotherapy treatment in dogs and cats is a much friendlier proposition for our fur babies compared to human anti-cancer therapies. To learn more, click here.
The prognosis for dogs and cats with primary lung tumors is variable, and has been shown to depend on several factors, particularly:
- Presence of clinical signs at presentation (poor)
- Size of the primary tumor (smaller is better)
- Tumor grade detected via biopsy (high grade worse than low grade)
- Evidence of metastasis (poor)
- Presence of cancerous fluid between the chest wall and lung tissue (called pleural effusion; poor)
- Tumor location in the lung lobe (peripheral location is better than a central one)
- Tumor adherence to the chest wall (poor)
In a study of cats with primary lung tumors, the median survival time for those without clinical signs was 578 days but only four days for those with clinical signs. In another study of dogs, median survival time was 15 months for those with non-metastatic disease treated only with surgery versus two months for those with lymph node metastasis. In general dogs with mostly good prognostic indicators have survival times beyond 18 months.
The take-away message about lung tumors…
Lung tumors affect our fur babies just as they do we humans. These lesions may arise from lung tissue (called primary lung tumors) or represent spread (metastasis) of a cancer in another location in the body (called secondary lung tumors). Early identification and surgical intervention of primary lung tumors is essential to ensure the best possible outcome. Partnering with board-certified veterinary specialists in internal medicine, surgery, and emergency/critical care will be invaluable in this endeavor.
To find a board-certified veterinary internal medicine specialist, please visit the American College of Veterinary Internal Medicine.
To find a board-certified veterinary surgeon, please visit the American College of Veterinary Surgeons.
To find a board-certified veterinary emergency/critical care specialist, please visit the American College of Veterinary Emergency and Critical Care.
Wishing you wet-nosed kisses,
cgb